As the population ages, the demand for hip replacement, knee replacement and other similar procedures will rise and patients will want new joints that last their extended lifespan, enabling them to enjoy an active old age.
Also impacting on the demand for joint replacement is the increase in obesity. Statistics from the National Joint Registry indicate that the number of joint replacement operations has been steadily increasing over the past few years, with the number of hip and knee procedures growing from 131,734 in 2005/06 to 163,940 in 2009/10.1
Products used to be available in sizes 1-5, for example, and you would pick the closest. Now you can adjust the individual sizes to match the natural kinematics of the patient, so the joint should last longer
The sector has been further impacted by the publication in April 2010 by the Medical and Healthcare products Regulatory Agency (MHRA) of an alert regarding possible soft tissue reactions to metal on metal (MoM) hip replacement devices. While it acknowledged there is likely to be no negative impact for the majority of patients, it warned that: "A small number of patients implanted with these hips may, however, develop progressive soft tissue reactions to the wear debris associated with MoM articulations. The debris can cause soft tissue necrosis and adversely affect the results of revision surgery."
The organisation recommended that patients be followed up for five years after undergoing the procedures and, where they are suffering with painful hip replacements, as well as for certain groups of patients, it advises health providers to consider measuring cobalt and chromium ion levels in the blood and/or cross sectional imaging in order to determine whether revision surgery is necessary.
More flexibility
According to Trevor Bailey from Orthodynamics, which is part of Summit Medical, there are various ways that products have been developed to achieve longevity in joint replacement. One of these is more flexibility in sizing. "Products used to be available in standard sizes and shapes and you would pick the closest size to match the patient," he explains. "Now you can adjust the individual sizes to match the natural kinematics of the patient, so it should give better performance and could last longer."
Orthodynamics UK's main product is CannulokPlus, a modular hip revision prosthesis with an interlocking intramedullary nail. Available in four stem diameters (11mm, 13mm, 15mm and 17mm) and a range of lengths, the system can be used 'off-the-shelf' or customised to fit the patient. In addition, the company says: "Multiple revision operations inevitably lead to the loss of proximal bone stock, particularly when associated with cement removal. The CannulokPlus solution allows effective distal fixation, allowing recovery of proximal bone stock over time."
Another company that has done a lot of work on materials to encourage bone ingrowth, is Corin Group. It has developed Bonit, a cementless, bio-active calcium phosphate coating with a microcrystalline structure which promotes bone integration. "Its biphasic composition enhances short and long-term osseointegration while the bone-like (biomimetic) coating morphology provides a potent capillary effect on blood accelerating the implant healing process," a spokesman said.
In addition, to address reactions to metal implants, Corin's replacement hip joints are coated with titanium nitride (TiN) ceramic, which, the company says, acts as a barrier to metal ion release, making it suitable for patients with allergic sensitivities.
Improving outcomes
Another challenge when fitting replacement joints is alignment, according to Phil Cleary from B Braun Medical. This is particularly important in knee replacements - the focus of B Braun's OrthoPilot technology. OrthoPilot uses an infrared camera tracking system to ensure the new joint is aligned correctly. Sensors are placed on the patient's femur and tibia, which send signals back to the camera. This enables the surgeon to place the joint without the need for X-ray, MRI or CT during surgery. "The system provides constant feedback," Cleary says.
Multiple revision operations inevitably lead to the loss of proximal bone stock, particularly when associated with cement removal
The OrthoPilot was developed about 12 years ago by Frederic Picard, a consultant orthopaedic surgeon at Glasgow's Golden Jubilee National Hospital and has resulted in a significant improvement in outcomes. "A lot of data says that the average orthopaedic surgeon gets it right only around 80% of the time, but with OrthoPilot the success rate is 98% ±3°, according to gate analysis on navigated knees conducted at the Golden Jubilee," Cleary explains.
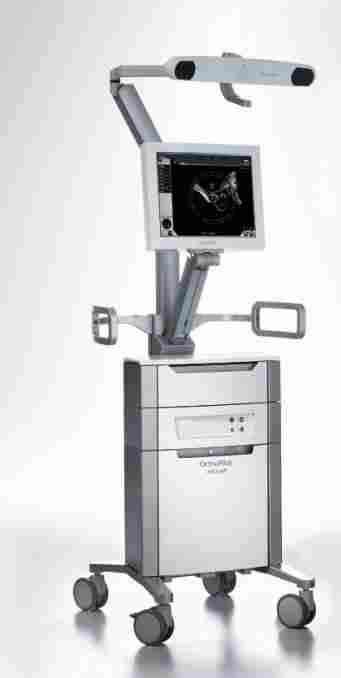
He added that, although the OrthoPilot was mainly developed for knee replacements, it also has potential for a wide range of other procedures including ACL ligament reconstruction, tibial osteotomy, hip replacement, sports medicine and revision knee surgery.
Stryker has also developed a system to improve the outcomes of knee replacement surgery - OtisMed ShapeMatch technology. Using proprietary 3D imaging software it builds a model of the patient's knee joint, which can then be used to fit the prosthesis. The technology works together with Stryker's Triathlon Custom Fit Knee to enable surgeons to position the femoral component according to the patient's flexion/extension, tibial rotation and patella axes in order to restore their unique joint kinematics. The company cites studies which have shown that its knee system provides the potential for greater stability throughout the range of motion2,3, improved motion4, more rapid return to functional activities4 and a better fitting implant5 for the individual patient.

Already in use in a number of centres in the UK, the technology will have its formal UK launch at the British Orthopaedic Association's annual conference in September. These are only a few of the advances in joint replacement technologies that have transformed accuracy, fit and longevity. Most have been in use for many years and have already gained the confidence of orthopaedic surgeons around the country. But the companies that produce orthopaedic technology continue to work on processes and materials that make the products easier to use and deliver greater benefits to patients.
References
1.National Joint Registry, Annual Report, 2010, Figure 1.6, Proportion of reported procedures by type of provider, 2005/06 to 2009/10
2. Wang, H., Simpson, K.J., Ferrara, M.S., Chamnongkich, S., Kinsey, T.,Mahoney, O.M. Biomechanical Differences Exhibited During Sit-To-Stand Between Total Knee Arthroplasty Designs of Varying Radii, The Journal of Arthroplasty, Vol. 21, No.8, 2006.
3. Designed to maintain collateral ligament stability throughout the range of motion. Stryker initiated Dynamic Computer Simulations of Passive ROM and Oxford Rig Test, Stephen Piazza, 2003
4. Harwin, S.F., Hitt, K, Greene, K.A. Early Experience with a New Total Knee Implant: Maximizing Range of Motion and Function with Gender-Specific Sizing Orthopedic Surgery, Surgical Technology International, XVI. pgs 1-7
5. Hitt, K., et al. Anthropometric Measurement 2003




